Sitting at the kitchen table rolling a ball of Play-Doh, Oliver Campbell is a image of childhood contentment. At just underneath two many years old he is experimenting with words and is happily peppering his innovative endeavours with them. But inside Oliver’s head something extraordinary is taking place. Currents from tiny electrodes, curled within the snail-shaped cochlea of his inner ear, are stimulating his auditory nerve, making it possible for him to hear the thud of the Perform-Doh and the creak of the chair and to assimilate the phrases of encouragement from his grandmother following to him.
Take them away and Oliver’s globe would be thrown into confusion.
Diagnosed with auditory neuropathy spectrum disorder (ANSD) at barely 24 hrs previous, Oliver was born unable to make sense of the sounds close to him. For his mothers and fathers, Chris and Claire Campbell, it was devastating.
Lightning, they realised, had struck twice. 5 many years earlier Oliver’s sister, Alice, was also born with ANSD – even though it took virtually 18 months for the diagnosis to be offered. “It was a massive shock,” Claire says. “There is no historical past of deafness at all in both side of the loved ones.” Certainly the couple’s 1st kid, Joseph, has no hearing troubles at all. But when Alice did not seem to be to be studying to speak as her older brother had, the Campbells knew one thing was incorrect.
The diagnosis was a bombshell. “Each and every hope and dream that you’ve ever had for this tiny youngster sitting in front you will get blown out of the water,” says Claire.
For Alice and her younger brother, anything in their ears had gone badly awry. And it was going to consider surgical treatment, education and some seriously hi-tech kit just before the clattering, chattering, bustling planet would come alive.
Hearing is a sense most of us take for granted, but in actuality it resembles a convoluted, anatomical version of the board game Mousetrap, played out within the fiendishly intricate architecture of the ear.
The ball is set rolling when sound waves arrive at the outer ear and are funnelled down the ear canal in which they end up banging into the eardrum. The vibrations from the eardrum move a small linked bone called the hammer, which is hooked up to more biological ironmongery in the kind of the anvil which is linked to the stirrup. The latter rests towards part of the inner ear which prospects on to the spiral-shaped cochlea.
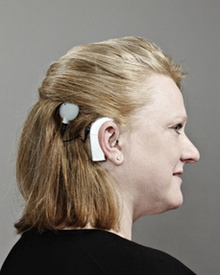
 Alice Campbell, who like her brother Oliver was born with auditory neuropathy spectrum disorder (ANSD). Photograph: Suki Dhanda for the Observer
Alice Campbell, who like her brother Oliver was born with auditory neuropathy spectrum disorder (ANSD). Photograph: Suki Dhanda for the Observer
And it is inside the cochlea that factors get technical. As the stirrup vibrates, it brings about fluid inside of the inner ear to move back and forth – motion that is picked up by a membrane and passed on to tiny hair cells within the cochlea. When the hair cells waggle, they release chemical compounds acknowledged as neurotransmitters that set off electrical impulses in auditory nerve fibres near by. These signals whiz along the auditory nerve to the brain where they are deciphered. Possibly remarkably the hair cells, and hence auditory nerve fibres, are laid out like a piano keyboard – those in the outer component of the cochlea’s spiral respond to high frequency sound, even though those close to the tight curl at the centre react to reduced frequencies.
There is no doubt it’s a complicated set-up, and one particular of evolution’s finest achievements. But when something goes incorrect, the consequences can be devastating. For Oliver, Alice, and a lot of other individuals, the dilemma was found in the cochlea. While ANSD is a broad phrase encompassing a range of brings about, and symptoms that can differ in severity day-to-day, the upshot is that sound waves attain the hair cells, but are then scrambled into an incoherent signal or fail to be turned into electrical signals at all. But cochlear implants can make a planet of difference. “For us it boiled down to a black and white determination,” Claire says. “It was, if you want your child to have hearing this is your only hope.”
Boasting an array of extremely sophisticated technologies, these implants have unsurprisingly been named “bionic ears”. Their staggering capacity to develop a sense of sound is down to a flexible electrode array that is gently nestled inside the cochlea during surgery. Finer than fishing twine, these wires let the typical auditory pathway to be sidestepped, shifting the lives not only of those with ANSD, but also individuals with the missing or broken hair cells or a broken auditory nerve typical of “sensorineural” hearing reduction.
Let’s reset the Mousetrap. Now sounds are picked up by an external microphone, hooked over the ear, and turned into a digital “score” of electronic stimulation patterns by a processor. This info is then transmitted wirelessly across the scalp, together with a dose of energy, in which it is picked up by a coil underneath the skin and passed to the implant exactly where the digital score is converted into electrical pulses. These are sent to the electrodes inside the cochlea, exactly where they artificially trigger electrical impulses in the auditory nerve fibres, bypassing the position of the hair cells. But although each and every hair cell stimulates only a handful of of these fibres, the electrical pulses of a cochlear implant set off much bigger areas. It really is a bit like enjoying a piano with giant hands – massive bunches of keys get hit all at when. But, wonderfully, the mechanism performs. It truly is elegant, it’s sophisticated, and it changes lives.
“You can see it first factor in the morning when Ollie initial puts his ears on,” Claire explains in excess of the sound of her son happily enjoying. “The noise commences coming and he sort of brightens up and lightens up and you know his globe is considerably far more open.” The engineering has also enabled Alice to attend a mainstream hearing college, learn to perform the drums and appreciate listening to music – her favourite tunes getting a blend of Queen and hits from Annie. It truly is been a long journey for the Campbells, and 1 that has been intimately shared by way of their website Alice’s Ears. But their hopes and dreams have returned. “Alice is flying now at college,” says Claire. “I am so proud of her and I’m so surprised by the technology and what it has offered her.”
Nevertheless it is technologies that, practically forty many years in the past, barely seemed possible. “In the quite starting there was a whole lot of scepticism, mostly by neurophysiologists,” reveals Professor Ingeborg Hochmair when we meet in the swish surroundings of the Med-El innovation centre in Innsbruck, Austria. “They couldn’t think it could function to stimulate just a couple of places in the cochlea, and by stimulating all around eight to twenty or so areas change the perform of 25,000 nerve fibres which there are in a regular auditory nerve, ” she says. “But it works.” As CEO of Med-El, a single of the biggest cochlear implant companies globally, Hochmair is recognised as a pioneer of the engineering – an accolade that final yr noticed her share the Lasker prize, an worldwide award in the field of medical study.
The new innovation centre, a futuristic-seeking development opened just final 12 months, is a testimony to the good results of her vision and challenging perform. But the procedure of constructing a cochlear implant is also impressive. Peeking through into the clean rooms, I see a host of figures in gowns and masks busily peering down microscopes, meticulously inspecting the laser welding of person implants or checking a silicone seal is excellent. Number of parts of the approach are automated, and it is claimed that if a consumer tells the firm the variety of their implant, Med-El can pinpoint the folks who constructed it. It really is a handmade device for a really individual application.
 Anita Grover: ‘I would not want to be in a social predicament for concern of missing element of the conversation.’ Photograph: Suki Dhanda for the Observer
Anita Grover: ‘I would not want to be in a social predicament for concern of missing element of the conversation.’ Photograph: Suki Dhanda for the Observer
And it is a trigger to which Ingeborg Hochmair has devoted her life. Possessing made the decision at just 13 years outdated that she needed to pursue a occupation in biomedical engineering she went on to review electrical engineering in Vienna. It was there that she and her future husband, Erwin Hochmair, grew to become involved in the nascent discipline of cochlear implantation. Functioning with researchers, surgeons and, crucially, patients, they soon notched up an extraordinary list of successes, and in 1990 started employing workers at Med-El. “As inventors we desired to see this become available for prospective end users,” she says. At the time each have been employed in academia, which Ingeborg later left to head the increasing firm. She believes their mutual passion for the technological innovation has contributed to her achievement. “This is a really fortunate constellation,” she says of the partnership.
But while the engineering has produced in leaps and bounds, Hochmair believes there is more to do. “There are even now so many young children that still have no entry to the technologies in numerous nations.” And fiscal outlay is not the only cause. “It really is awareness: numerous families just don’t know about that probability. It really is infrastructure in some nations,” she says.
With children, it is a race towards time. For these born unable to hear, it is vital to implant the units at a younger age, ideally just before two years outdated and ideally nearer 9 months, to maximise the child’s capacity to produce speech, language and listening skills. With out the input of auditory signals, the brain does not fully develop the capacity to decipher sound, and as time ticks by this capability for adjust – acknowledged as plasticity – decreases. What is far more it has been advised that, if unused, these locations of the brain steadily become reassigned to tackling other tasks.
Even with a cochlear implant, there are even more hurdles to encounter in harnessing the engineering. “Somebody informed me once that [having] a cochlear implant is a bit like becoming handed a important to a Porsche and not understanding how to drive,” says Anita Grover. “The brain has access to all this sound but it has to really understand to make sense of it.”
As chief executive of Auditory Verbal United kingdom , a charity that provides therapy to youngsters receiving to grips with their bionic ears, Grover is passionate about assisting other people to make the most of the engineering. “I would like all kids whose household needs them to be in a position to listen, speak and accomplish to have accessibility to auditory verbal therapy to support them maximise the prospective of their cochlear implants,” she says. “There is a very tiny window in which there is plasticity in a younger brain, which implies there is a real chance to maximise the improvement of listening and spoken language. If you get the early intervention right with the correct engineering and habilitation then you get the possibility for deaf children to realise their potential. And that likely must be the very same as a hearing child.”
Grover is effectively acquainted with the technology. Possessing knowledgeable progressive hearing reduction, by her late 20s hearing aids have been no longer helping. As a civil servant she had relied heavily on lip-studying, but it was far from ideal. “I would be in a meeting [with] 15 to 20 folks around the table and it was like Wimbledon,” she says. “It really is so extremely tiring – you have acquired no backup.” In the end, a cochlear implant became essential. “With no a cochlear implant I hear nothing at all, absolutely practically nothing,” she says. “It changed my lifestyle. I had gone via that approach of my hearing deteriorating whereby I was becoming more and a lot more withdrawn. I would not want to be in a social situation for fear of missing component of the conversation or something possessing been mentioned, or possibly getting the pitch incorrect – shouting in a quiet spot or becoming quiet in a noisy spot.” And there are sounds you would never want to miss. “When the first of my twins was born he came out screaming,” says Grover. “I would not have heard that if I didn’t have a cochlear implant.”
But adults are in danger of becoming overlooked. Recent figures from the charity Action on Hearing Reduction reveal that a single sixth of the UK’s grownup population have some type of hearing issues even though a 2013 research suggests only 5% of grownups whose lifestyle could be enhanced by cochlear implants truly obtain 1. “For adults, I would like to see improved access to at least a single implant and ideally two,” says Grover.
It truly is the dark side of the accomplishment story. Policy launched in 2009 by the National Institute for Well being and Care Excellence (Nice) dictates that although kids deaf in the two ears ought to obtain two implants as a matter of program, adults are permitted only 1 – except if they have a 2nd disability, such as blindness, that can make them more reliant on hearing. It is an concern that Labour MP Lilian Greenwood place squarely to the Home of Commons in November. “A increasing physique of evidence indicates that bilateral implants offer extra enhancements in speech perception in noisy environments in excess of unilateral implantation, and much better sound localisation, foremost to improved good quality of existence,” she said.
Azhar Shaida, consultant otologist and cochlear implant surgeon at the Royal National Throat, Nose and Ear hospital agrees but says: “The problem is down to money versus advantage.” With the assessment, implant, surgical procedure and a year’s therapy costing £38,000-£45,000 for a single implant it’s an high-priced business, though with discounts obtainable on a 2nd gadget and only 1 hospital procedure necessary if implanted simultaneously, the expense of bilateral implantation is not double the value. Even then Nice doesn’t believe the advantages enhance quality of existence ample, in contrast with the existence-altering result of the very first implant, for adults to merit the cost.
 Stuart McNaughton: ‘I pushed for two years [for] the NHS to give me the 2nd one.’ Photograph: Suki Dhanda for the Observer
Stuart McNaughton: ‘I pushed for two years [for] the NHS to give me the 2nd one.’ Photograph: Suki Dhanda for the Observer
Customers this kind of as Stuart McNaughton, a lecturer at Westminster Enterprise School who also works for cochlear implant firm Sophisticated Bionics, say grownups deserve greater. “I pushed for two many years [for] the NHS to give me the second a single,” he tells me over coffee amid the bustle of Waterloo station. “Due to the fact I educate, element of my livelihood is extremely dependent on my ear working and, you know, occasionally items go wrong and if the 1 ear that you’ve got goes incorrect you lose your livelihood.” Fundamentally, he says, it is about going through the world individuals of us who can hear consider for granted. “It can make me the way I should have been, the way you are.”
But McNaughton is one particular of a small group of adults with bilateral cochlear implants. And like Greenwood, he believes it is substantial time attitudes in direction of grownups transformed. “I understand that young children want far more input simply because they are establishing language and they are creating expertise, but what about all the individuals more than the age of 18, 19, twenty, 21? They need to be allowed bilateral implants as well. Society puts pressures on grownups too – relationships, jobs – it’s a rat race out there.”
It truly is a contact to arms that resonates across the health-related occupation. As Shaida explains: “Two ears are better than one. Two cochlear implants are far better than 1.” The situation is particularly desperate for individuals who have suffered from meningitis. “With meningitis you often get obliteration of the cochlea,” he says. “Normally for the meningitis sufferers we fast track them so that we can get the implant in as quickly as achievable before the cochlea gets to be totally blocked and it is extremely hard to do an operation.” For such patients simultaneous bilateral implantation could be crucial. “If we came back later on to implant the other side due to the fact the first side had failed, it [could not] be possible simply because of the blockage.”
But the 2009 Nice guidelines make it clear: even in this kind of conditions simultaneous bilateral implantation is basically not an selection.
The introduction of the recommendations has also fuelled fears of deepening inequalities. “What we are seeing is a quantity of patients are opting to have one particular completed on the NHS and getting the 2nd one carried out privately. Which is excellent – if you can afford it,” says Shaida.
David Selvadurai, consultant otolaryngologist surgeon at St George’s hospital, London, also believes it is time for alter. “As a local community of experts we are keen to push this forward and we would like to see bilateral implants in grownups turn out to be far more acceptable,” he says.
But with the guidelines only reviewed every couple of years, he believes timing is almost everything. “What we do not have at the minute is good value benefit data to show that there’s adequate advantage to the personal to demonstrate value effectiveness for the NHS,” he says. “The danger that we have to be wary of is that the recommendations are reviewed ahead of the needed evidence is accessible.”
It truly is a scenario Shakeel Saeed, professor at UCL and the Royal National Throat, Nose and Ear hospital is determined to adjust. Working with colleagues at the Ear Institute, he is presently scoping a nationwide, multi-centre potential review on bilateral cochlear implantation in adults. “This is to create higher good quality proof that Nice can then use to make a considered choice.” Gathering the proof, he says, will take 4 to 5 years – and it will not be inexpensive. But it is a possibility they can’t afford to miss.
“If we complete that review then we will be ready to solution a quite straightforward query: does the benefit of having two implants in adults justify the value?” says Saeed. “We might find it doesn’t – but I suspect that we will find that it does.”
Bionic ears are a technological triumph. It’s time adults, like youngsters, had been permitted to expertise the complete measure of their metamorphic possible.
Bionic ears: let us hear it for cochlear implants…





