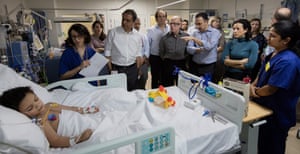
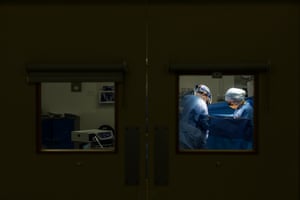
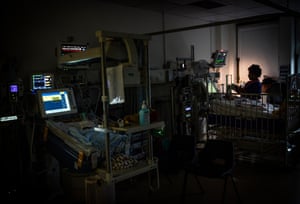
Electroconvulsive therapy is such a serious treatment that there is something almost prosaic about the place where it happens. There is a sense that the therapy is no more dramatic – or time-consuming – than visiting a blood bank. There is even a tea and biscuit station at the end.
Within a suite of five rooms at the Barnet, Enfield and Haringey Mental Health NHS trust, classical music floats across the airwaves casting an uplifting atmosphere over the standard hospital decor of blue lino, magnolia walls and no-nonsense chairs.
Robert Tobiansky, the lead ECT consultant, talks us through a typical procedure.
“We treat anywhere between 30 and 50 patients per year and it has been like that for as long as I have been around,” he says, adding that numbers for the clinic, held twice a week, vary throughout the year. “Our list today was five – we have been very busy lately.”

We pass through a small waiting room and then an office-like space where each patient is talked through the process of ECT and asked for their consent.
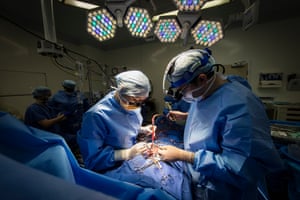
Next is the treatment room, a clinical space with one trolley bearing anaesthetic equipment and another carrying the ECT machine.
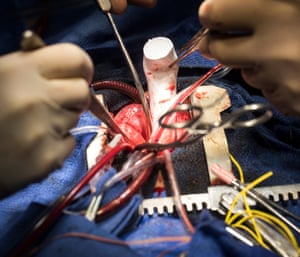
“It might not look like much, but that blue box cost 25 grand,” says Tobianksy. He picks up the electrodes, or paddles – each about the size of a coffee jar – and demonstrates how they are placed on a patient’s head.
The machine is also connected to what appears to be a jumble of cables. These, says Tobiansky, are for monitoring the patient’s brain activity throughout the procedure. “As well as being able to give an electric stimulus, in such a way that it is giving minimal amounts of electricity but sufficient to induce a seizure, it also monitors the duration of the seizure,” he explains.
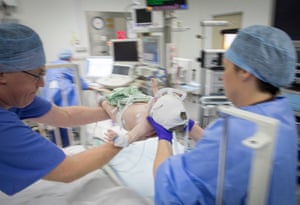
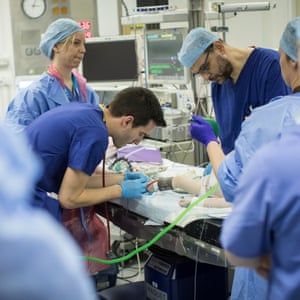
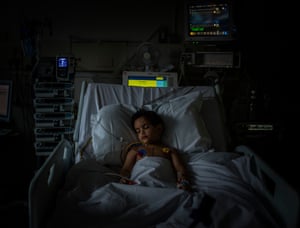
After lying down on a trolley the patient is given an anaesthetic and muscle relaxant, with blood oxygen and heart rate monitored. The paddles are then placed on their head and a current applied for just a few seconds – inducing a short seizure.
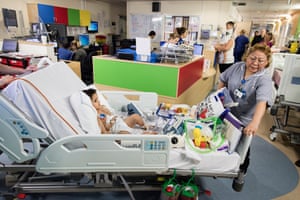
A stint in the recovery room follows – an airy space with four beds each bearing a green mattress and yellow pillow. On the walls are paintings, while blue blinds are half drawn at the window.
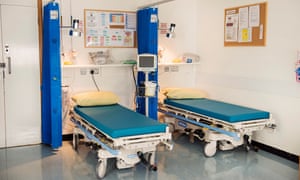
Typically, says Tobiansky, patients are a little groggy, perhaps with a headache or nausea as they come round. “We check how quickly people become re-oriented by asking: ‘Do you know where you are? Do you know the date?’ etc, and we are documenting how long that takes.” Within 15 minutes most patients are back on their feet.
The final room contains a kettle – patients are offered tea or coffee and a biscuit before they leave the suite, an important step since the general anaesthetic means they have had to fast for six hours prior to the treatment.
Typically, says Tobiansky, ECT is used to treat patients with severe depression, often accompanied by psychotic symptoms, a high risk of suicide or a refusal to eat or drink.
“This is somebody who through their depression feels that they are not worthy of eating or drinking, who through their illness is starving – that is a life-threatening condition,” says Tobiansky. “You have not got time to wait for other things not to work. Likely things have been tried and failed.”
But, he adds, negative, dramatic depictions of the treatment in film and other media have left their mark. “Although it is small numbers of people who have the treatment we usually have a big battle against the stigmas and the very negative press ECT has,” he says.
While Tobiansky admits ECT can cause memory problems, and it is difficult to predict to what degree that will affect each patient, he says there is no evidence that it causes brain damage or dementia.
“I have seen it help so many people over so many years where nothing else has helped them,” said Tobiansky.
“In my opinion, ECT is underused. [But] it is not a panacea.”
Tea, biscuits and classical music: inside an ECT clinic