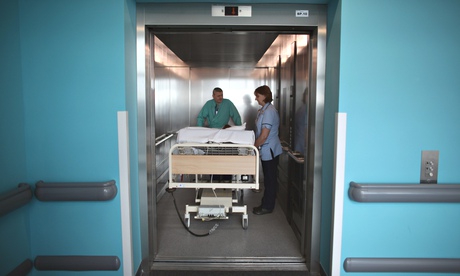
The case of Iris Sibley, trapped for six months in a Bristol hospital while her family and health authority hunted for a suitable care home, has highlighted how “bed blocking” is a key term in the crisis currently engulfing the NHS. When this week brought the news that nine out of 10 hospitals are overcrowded, NHS bosses pointed to major problems discharging patients. A&E’s failure to meet its four-hour target has similar causes and the excellent BBC TV series Hospital has highlighted how operations, both urgent and routine, are being delayed because beds needed for recovery are “blocked” by patients who no longer need to be in hospital.
Bed blocking is an impersonal term that expresses hospitals’ problems with resources. For the patients and family, it is much more personal. My mother became a “bed blocker” three years ago when, aged 89 and suffering from dementia, she collapsed and was admitted to hospital. She’d had several hospitalisations in the previous eight years but on the other occasions she’d been patched up and returned home. This time, after two weeks, she was declared stable but unable to cope any more on her own. I was told that a care home should be found, and rather sheepishly that the hospital “needed the bed back”.
We found a home within four weeks, yet it was another month before my mother was discharged
Like our society facing the coming crisis in elderly care, I wasn’t in any way prepared for this moment. Every time my mother had been hospitalised previously we’d seen first-hand what was being cited as the reason for much bed blocking: hospital weakened her, medication was altered, and her social care fell apart and became more difficult to re-establish as cuts hit social services. But in spite of all these mini-crises, we usually managed, eventually, to get her home. This time we had to make alternative arrangements.
The following five weeks were terrible. I was very distressed. I felt guilty. I had nightmares about making my mother leave her home. Contrary to Tory minister David Mowat’s recent comments that families aren’t prepared to care for their elderly parents at home, I clung to the hope that we could find a halfway house to rehabilitate her, or we could find additional social care to keep her at home. But the hospital kept pressuring and I shifted to scouring care homes and taking a crash course in what had become an overwhelmingly important issue: how a care home would be funded.
This was a lot of work, but ultimately it wasn’t me who held things up. We found a home within four weeks, yet it was another month before my mother was discharged. It is hard to pin down exactly why, but in the mix were cancelled meetings with consultants, staff absences and a lack of continuity between various agencies.
Worst of all was the finances. Endless time was spent researching funding and working on the care assessment form that determines the NHS’s contribution to care out of hospital. Despite huge numbers of older people now needing “medicalised” care of the sort previously provided in geriatric wards by the NHS, they are not entitled to full funding in care homes. But getting to the point of understanding entitlements and contributions and being therefore able to finalise the care home arrangements is a struggle. The eventual verdict had been anticipated by the discharge nurse five weeks previously: my mother was entitled to the basic further care element and the rest she would have to pay for herself, with the proceeds of selling her home.
Just as we began to gently prepare my mother for the move, she was abruptly shifted to another ward. She became extremely distressed and confused, and cried for the first time since entering hospital. And her whole care team disappeared – all the people with whom we’d been making these decisions and negotiating finances. The cause of this was again a shortage of beds, but for a person suffering from dementia and who was about to make the most important move of her life, it was awful.
It is not the fault of the NHS staff. In this instance they were uniformly compassionate. But while the staff don’t lack compassion, the system certainly does. Older people needing medicalised social care shouldn’t be pawns in a bureaucratic game where beds, forms and financial targets take precedence over humanity, while the NHS and councils, responsible for social care, desperately try to get the other to shoulder the costs. It’s shameful that resources are so scarce for the care of elderly people that it feels like horse trading to get anything at all.
Care for older people needs to change urgently. When my mother became a bed blocker the promises of the 2011 Dilnot report hung in the air. Dilnot was trying to rationalise the system, cap families’ contributions, and encourage social insurance to fund elderly care properly. Years later I’m shocked to find that nothing has changed. Theresa May talks about making Britain “work for all”, but Dilnot’s suggestions, which could improve life for elderly people and their families, have dropped off the radar.
When my mum became a ‘bed blocker’, I saw the crisis in care for older people | Ros Coward